|
|
International Journal of Arrhythmia 2015;16(1): 59-64.
|


Introduction
Narrow-QRS tachycardia with a long RP interval presents interesting
diagnostic challenges. A correct diagnosis is essential for performing safe
and effective catheter ablation. The differential diagnosis of
narrow-QRS tachycardia with a long RP interval includes atypical
atrioventricular nodal reentrant tachycardia (AVNRT), ectopic
atrial tachycardia, and atrioventricular reentrant tachycardia (AVRT)
with a decremental property. I present a case of permanent junctional
reciprocating tachycardia (PJRT) with a long RP interval that exhibited a
decremental property.
Case
A 65-year-old woman was referred to our hospital for sustained
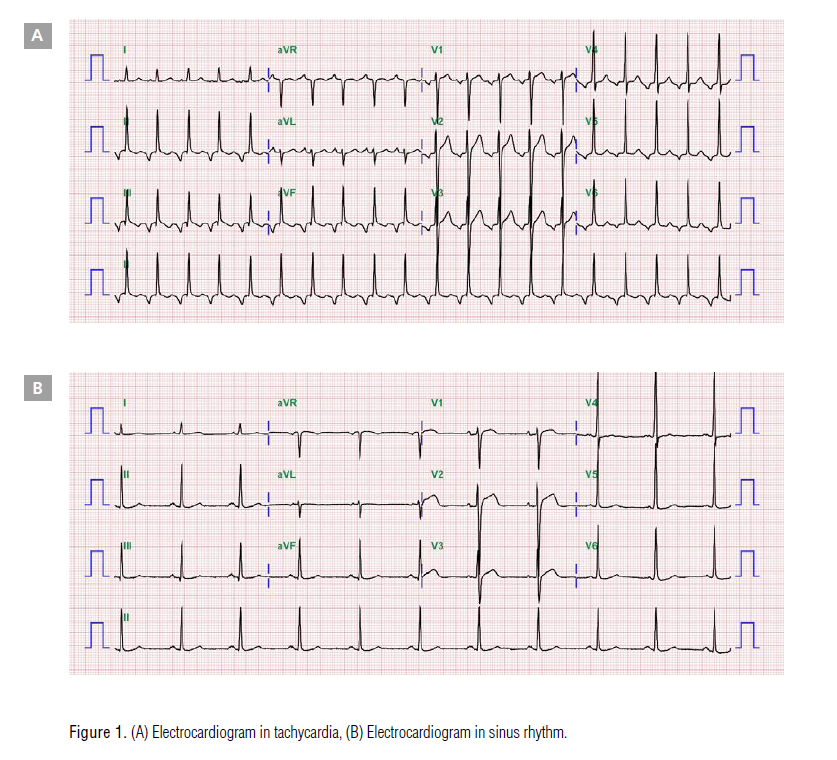
palpitations and general weakness. The electrocardiogram (ECG)
showed narrow QRS tachycardia of ~120 /min, with an inverted
P wave in leads II, III, aVF, and a long RP interval in all precordial
leads (Figure 1). She had normal left ventricular function on echocardiography, with an ejection fraction of 62%. Twenty-fourhour
Holter monitoring showed repeated induction of
supraventricular tachycardia (SVT), with intervening periods of
sinus rhythm lasting a few minutes. I administered IV adenosine,
verapamil injection, and DC cardioversion several times in an
attempt to terminate the tachycardia, but after few seconds in
sinus rhythm the tachycardia was reinduced and sustained. To
maintain sinus rhythm I prescribed 240 mg of verapamil or 150
mg of atenolol per os; however, the patient continued to exhibit
the same drug-refractory tachycardia.
The patient was scheduled for electrophysiological study and
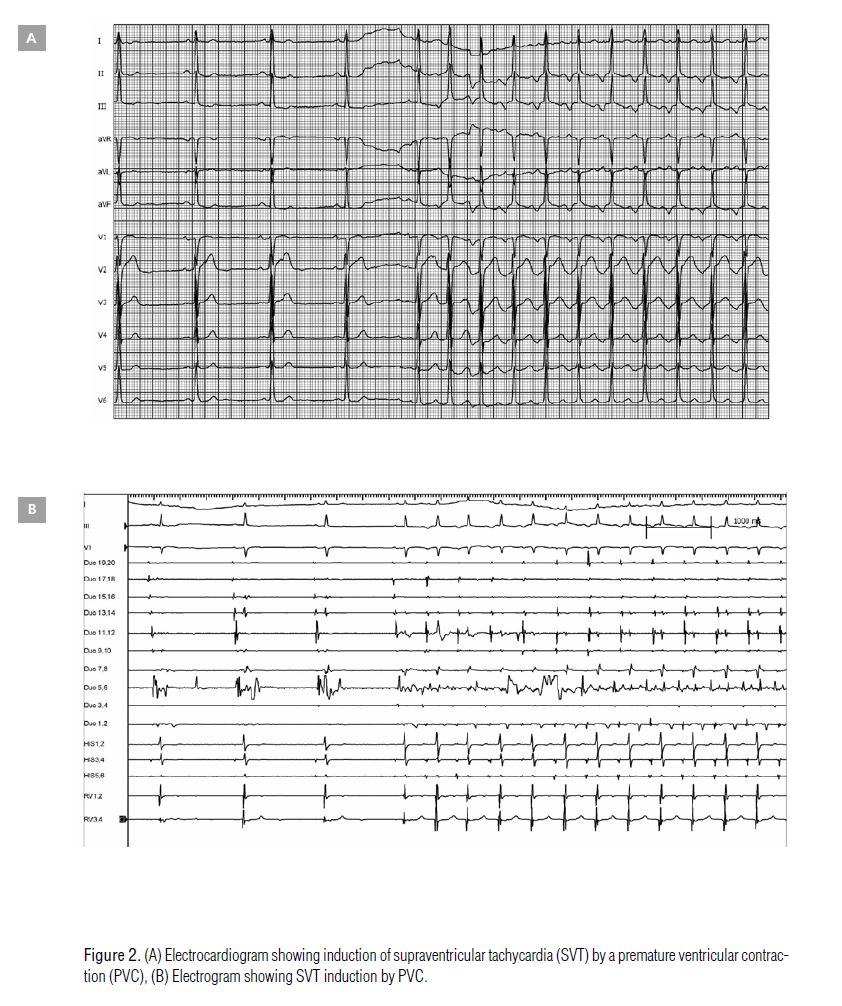
catheter ablation. In the electrophysiology lab she showed SVT
with intermittent short periods of sinus rhythm. The SVT could
be easily induced by one premature ventricular contraction
(PVC), and was also inducible in sinus rhythm without any AH
jump (Figure 2). For the differential diagnosis, I applied a PVC
during SVT. In contrast to orthodromic AVRT without a
decremental property, after the PVC the AA interval was
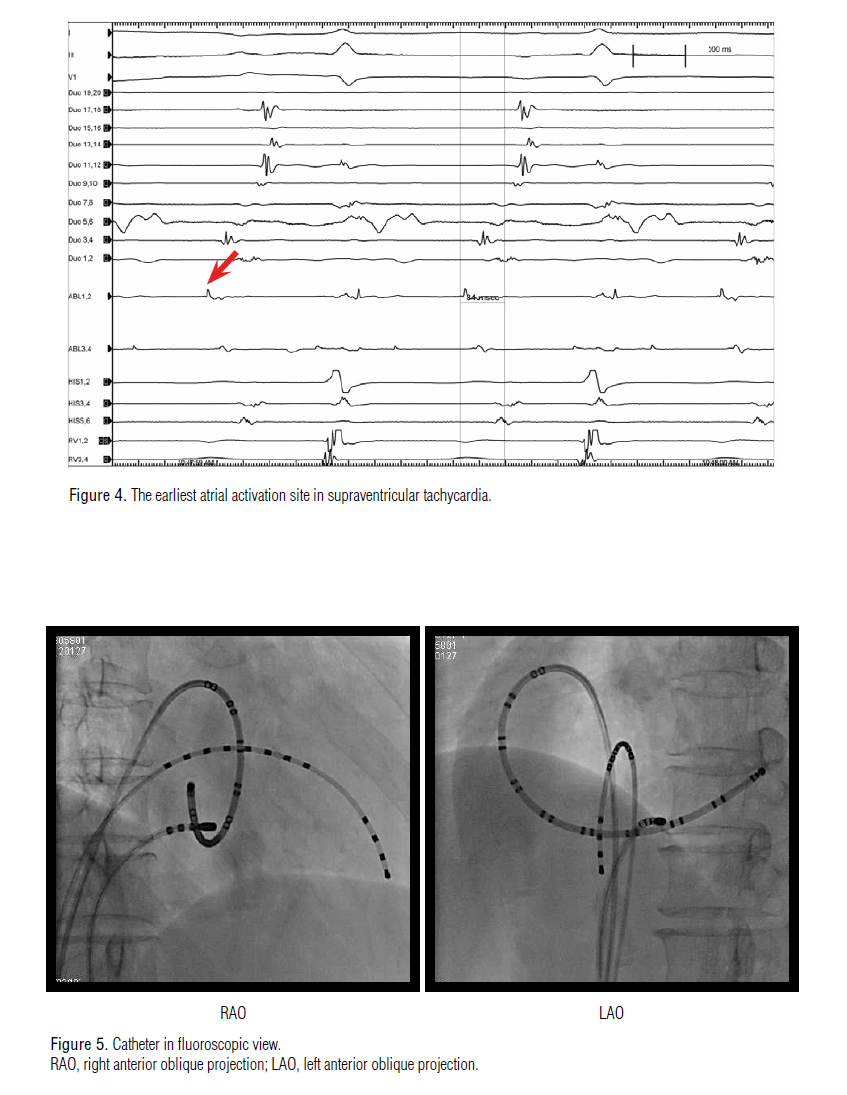
prolonged from 467 ms to 494 ms (Figure 3). To ablate the accessory pathway, I identified the earliest activation site of A in
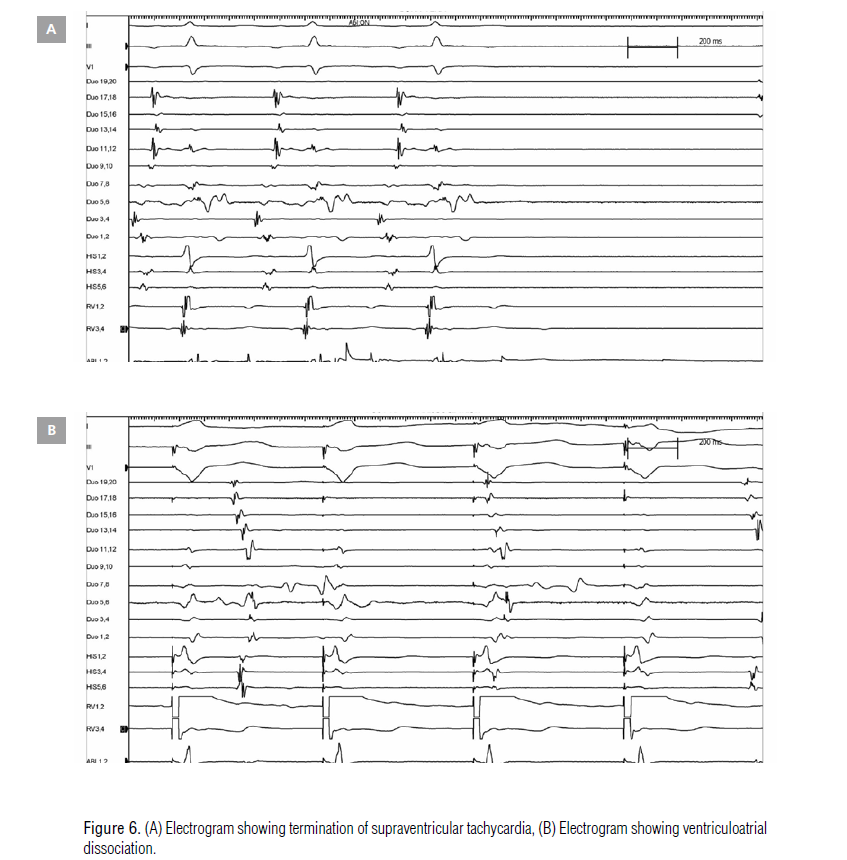
the right posteroseptal area (Figure 4, Figure 5). After 4 seconds of
radiofrequency application, the SVT terminated and showed
ventriculoatrial dissociation (Figure 6). The patient remained in
hospital for two days after the catheter ablation and was
discharged in sinus rhythm.

Discussion
In this case, no preexcitation was observed. During the
tachycardia, the earliest atrial activation was observed around the
coronary sinus ostium. The critical finding for the differential diagnosis was the atrial response to a PVC during the His
refractory period. Since the atrial activation was delayed by the
PVC, AVNRT could be excluded.1
PJRT is an orthodromic AVRT mediated by a concealed and
slow-conducting accessory pathway. The clinical course of PJRT is
not always benign. Many patients try multiple antiarrhythmic
drugs and ultimately require catheter ablation. Radiofrequency
catheter ablation is a safe and effective therapy.2 However, the
higher recurrence rate of PJRT, compared with that of reentry
with no decremental property, may be explained by the long,
tortuous course of the accessory pathway. The most important
complication of incessant PJRT is tachycardia-induced cardiomyopathy, which has been observed in 18% of patients with
PJRT.3 Slower conduction through the accessory pathway has a
wider excitable gap. In most cases of PJRT, the accessory pathway
is located in the posteroseptal region.
References
- Ho RT, Frisch DR, Pavri BB, Levi SA, Greenspon AJ. Greenspon. Electrophysiological features differentiating the atypical atrioventricular node- dependent long RP supraventricular tachycardias.
Circ Arrhythm Electrophysiol.
2013;6:597-605.
- Meiltz A, Weber R, Halimi F, Defaye P, Boveda S, Tavernier R, Kalusche D, Zimmermann M. Permanent form of junctional reciprocating tachycardia in adults: peculiar features and results of radiofrequency catheter ablation.
Europace.
2006;8:21-28.
- Bensler JM, Frank CM, Razavi M, Rasekh A, Saeed M, Haas PC, Nazeri A, Massumi A. Tachycardia-mediated cardiomyopathy and the permanent form of junctional reciprocating tachycardia.
Tex Heart Inst J.
2010;37:695-698.
|
|
|
|