Introduction
In patients with a dual chamber pacemaker, wide QRS regular tachycardia occurs under various conditions, such as sinus tachycardia, atrial tachycardia, and pacemaker-mediated tachycardia. Frequently, accurate diagnosis is difficult when P waves overlap large T waves. However, atrial fibrillation or atrial flutter is commonly detected by the automatic switching algorithm, and the DDD(R) mode is converted to the DDI(R) or VVI(R) mode when atrial fibrillation (AF) or atrial flutter (AFL) develops. In the present case, regular wide QRS tachycardia with fixed heart rate developed in the DDD mode. What is the mechanism?
Case
A 67-year-old male patient presented with a history of aggravated severe dyspnea for several months. A chest radiograph showed severe cardiomegaly, and an electrocardiogram revealed sinus tachycardia with ventricular paced beats. An echocardiogram revealed a large amount of pericardial effusion (Figure 1). He had been treated for chronic kidney disease over several years, and his serum creatinine level was 2.7 mg/dL.
A DDDR pacemaker had been implanted 2 years previously for complete atrioventricular block. Paroxysmal atrial fibrillation was diagnosed during follow-up, and he was treated with a class Ic antiarrhythmic agent (flecainide). He maintained sinus rhythm over 1 year.
To treat his pericardial effusion, pericardiostomy was planned. During surgery, the pacemaker mode was temporarily changed from DDDR to DOO at 70 beats per minute (bpm) to avoid electromagnetic interference. After drainage of a large amount of serous fluid, dyspnea was relieved, and the patient did not experience discomfort.
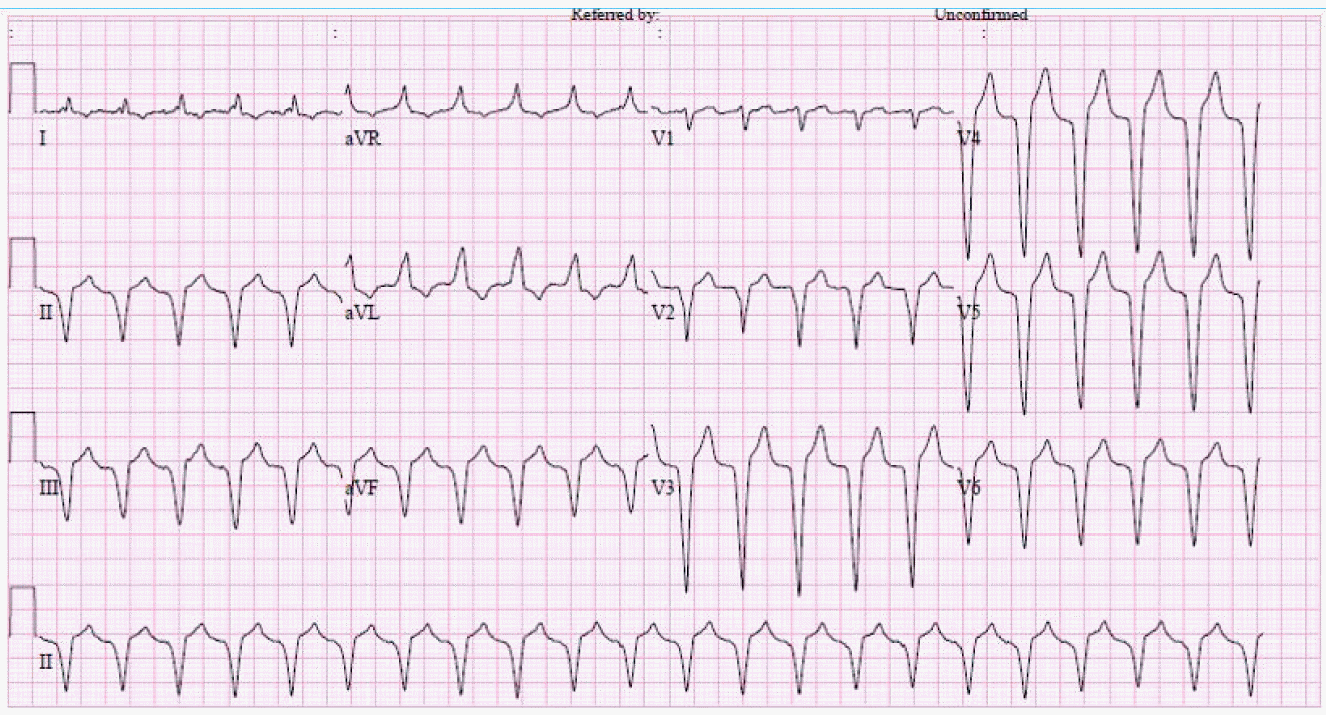
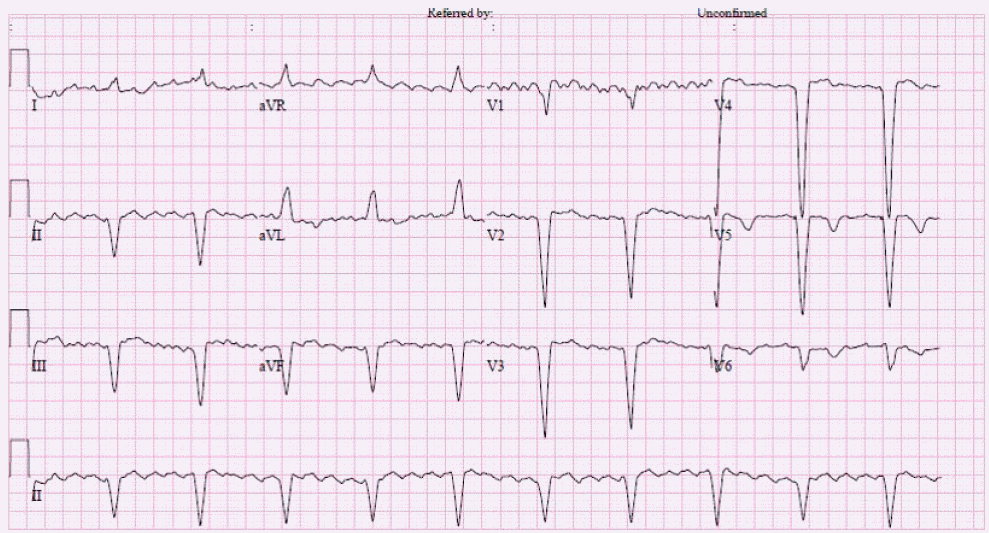
However, 2 days after surgery, the patient presented with chest discomfort and dyspnea. His heart rate was 150 bpm, and an elecctrocardiogram (ECG) showed paced ventricular rhythm (Figure 2). Sinus tachycardia associated with anxiety was assumed, but other tachycardias were considered because the rhythm sustained for more than 1 day at the same heart rate.
A chest radiogram and echocardiogram revealed that there was no aggravated pericardial effusion causing dyspnea.
Pacemaker interrogation was performed, and an intracardiac atrial electrogram (EGM) showed very fast regular rapid atrial tachyarrhythmia (Figure 3). Ventricular pacing was regular because the ventricular pacing followed every fourth atrial beat. The first three atrial activities were in the post-ventricular blanking period and post-ventricular atrial refractory period. After a total atrial refractory period, only a single atrial activity occurred at the sensing window, causing ventricular pacing. It was one explanation of regular ventricular response.
Generally, the pacemaker should have automatically switched the mode when atrial flutter developed, which would have helped in the diagnosis. However, when the DDD mode was turned on after surgery, the automatic mode switching function was mistakenly not activated.
After activating the automatic mode switching function, the ventricle was regularly paced at 60 bpm in the VVIR mode with atrial flutter waves (Figure 4). When atrial flutter on ECG was studied inrelation to the atrial activity on intracardiac EGM, it was observed that waves of atrial flutter almost matched every other atrial activity on EGM. The first and marked atrial activities of intracardiac EGMs were somewhat irregular or showed slurred wave pattern. Using these findings, marked atrial activities in intracardiac EGM were considered to be composed of atrial flutter of about 300 beats per minutes (bpm) and intervening electrical noises one after another. Ventricular pacing was performed after the last atrial flutter rhythm resulting in a ventricular rate that was half atrial flutter rate. Previous atrial sensed beats were ignored because they were in post-ventricular blanking (PVB) period and post-ventricular atrial refractory period (PVARP).
Sinus rhythm was restored by electrical cardioversion and the patient was stabilized and discharged.
Discussion
Atrial flutter is frequently observed in patients who are being treated with taking class Ic antiarrhythmic medication for paroxysmal atrial fibrillation. Atrioventricular (AV) nodal blocking agents such as beta-blockers and non-dihydropyridine calcium antagonists are used before class Ic antiarrhythmic agents are given to prevent rapid ventricular response to atrial flutter.
In patients who have AV block and are fitted pacemakers, AV nodal blocking agents are obviously ineffective. Therefore, the automatic mode switching algorithms have been developed to detect atrial tachyarrhythmias and convert the pacemaker mode to a non-atrial tracking mode such as VVI(R) or DDI(R) [1]. Although detection of atrial arrhythmias remains the greatest challenge for mode switching algorithms [2], the automatic mode switching algorithms are very useful in detecting the occurrence of atrial tachyarrhythmias in patients who are fitted DDD(R) pacemakers.
Mode switching during atrial flutter may not reliably occur because atrial activities (sometimes every other atrial activity) occur in a blanking period. Thus, in some cases, the programmable interval can be used for a special response to atrial flutter [3].
When atrial flutter occurrs, the ventricular rate could be very rapid if every flutter wave is followed by a ventricular paced beat. This happens in any kind of atrial tachyarrhythmias. PVARP is one of the pacemaker timing functions that starts with ventricular activity and acts on atrial channel and prevents the AV interval from restarting due to sensed events such as far-field R waves, retrograde conduction or atrial tachyarrythmias.
In this case, automatic mode switching did not function just by mistake, not by special response for AFL. In this patient, because atrial flutter wave appears just after PVARP whereas other electrical noises and previous flutter activity was within PVARP. Moreover, the upper rate limit had been set at 160 bpm; therefore, an atrioventricular Wenckebach response following the sensed rapid atrial activities did not occur. Frequently, the identification of P waves superimposed on large T wave is difficult, especially during tachycardia. When consistent regular tachycardia occurrs, atrial tachyarrhythmias such atrial flutter or atrial tachycardia should be presumed. Prompt interrogation of the pacemaker and intracardiac electrogram analysis are mandatory.