Introduction
Atrial fibrillation (AF) is a well-established complication of myocardial ischemia [1]. The pathophysiology by which AF develops in this setting is not completely understood. Recently, we experienced a rare case of immediate cardioversion from AF after successful revascularization in a patient with chronic total proximal right coronary artery (RCA) occlusion.
Case
A 72-year-old woman with hypertension and diabetes mellitus visited the outpatient clinic complaining of chest discomfort. Her electrocardiogram (ECG) revealed AF with rapid ventricular response and 1 mm ST-segment elevation in I, aVL, aVR, V4-V6 leads (Figure 1). Blood tests revealed normal cardiac enzyme levels. A 2D-echocardiogram demonstrated normal regional wall motion, good systolic function, and mild left atrial (LA) enlargement (size 42 mm). As she had a CHA₂DS₂-VASc (congestive heart failure, hypertension, age≥75 years, diabetes mellitus, stroke/transient ischemic attack, vascular disease, age 65–74 years, sex category) score of 5 points, she was commenced on oral anticoagulation and a β-blocker.
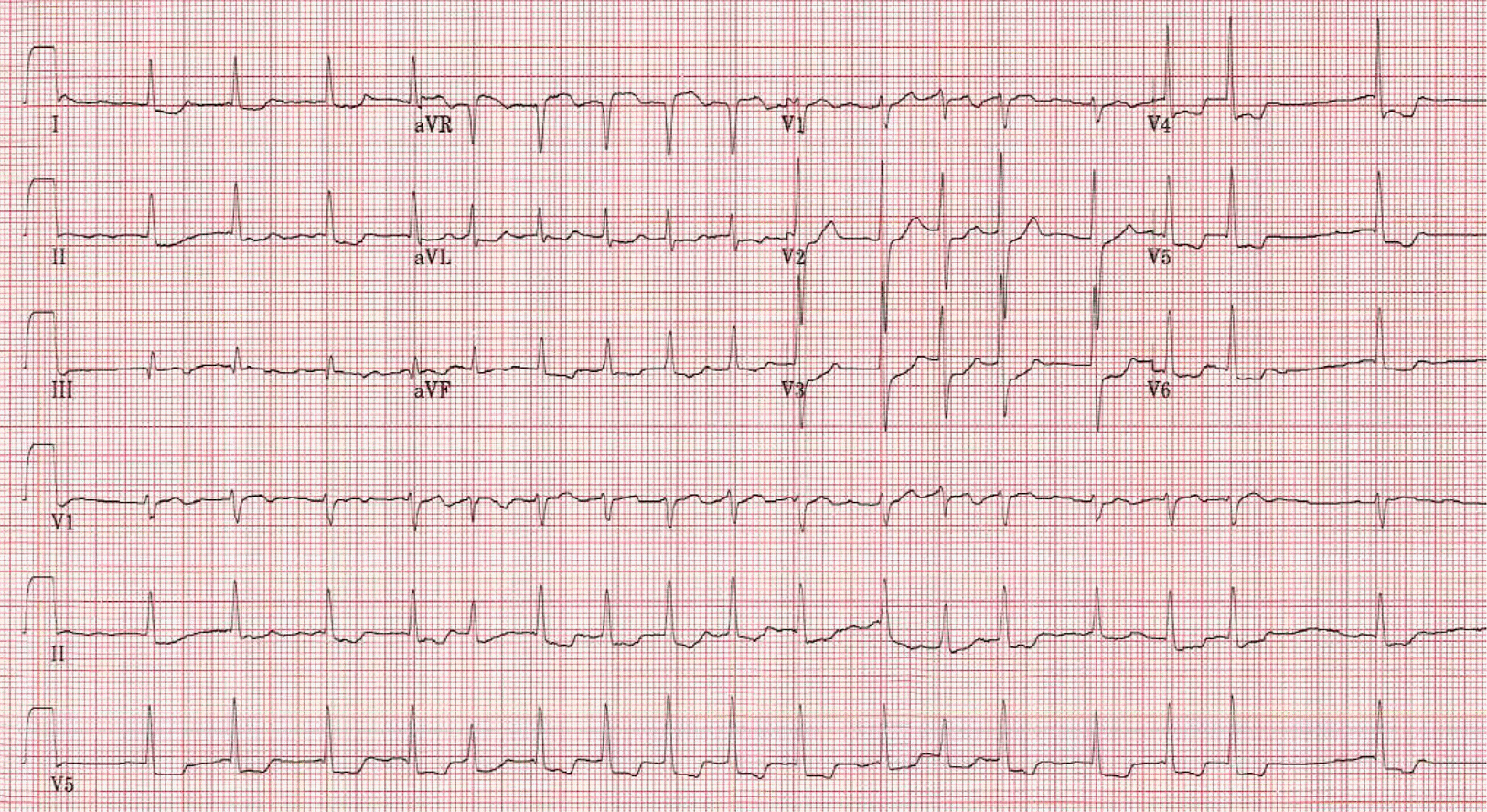
Figure 1.
12 lead electrocardiogram (ECG). ECG showed atrial fibrillation with rapid ventricular response and ST deviation in I, aVL, aVR, V4-V6.
Despite the administration of appropriate treatment for her AF, after 3 months, she continued to complain of intermittent substernal chest discomfort relieved by sublingual nitroglycerin therapy. She was referred for cardiac catheterization, which revealed total occlusion of the proximal RCA with grade III collateral filling of the distal RCA from the septal branches of the left anterior descending (LAD) artery (Figure 2). A discrete mid 80% stenosis of the LAD was also present. Coronary intervention targeting the RCA via an antegrade approach with a hydrophilic floppy wire (Fielder FC™, Asahi Intec, Japan) and a microcatheter (Corsair™, Asahi Intec. Japan) was performed. After several attempts, the guide wire was passed through the occluded lesion, and the lesion was dilated using a 1.0 mm, 2.5×15 mm balloon. The coronary angiogram then showed a thrombolysis in myocardial infarction (TIMI) grade III blood flow through the RCA, the sinoatrial nodal branch, the acute marginal branches and the atrioventricular nodal branch. The patient's cardiac rhythm reverted from AF to sinus rhythm immediately (Figure 3). The diseased segment was then further dilated to facilitate the placement of drug eluting stents: 4.0×20 mm Promus premier® (Boston Scientific, Natick, MA, USA) in the proximal RCA, 3.0×24 mm Promus premier® (Boston Scientific, Natick, MA, USA) in the distal RCA, and 3.0×20mm Promus premier® (Boston Scientific, Natick, MA, USA) in the mid-LAD.
Figure 2.
Coronary angiogram. A: Coronary angiogram (CAG) revealed chronic total occlusion of proximal right coronary artery (arrow). B: CAG revealed significant stenosis in mid left anterior descending artery (LAD) (black arrow) and grade III collateral filling of the distal RCA from septal branches of LAD (white arrow).
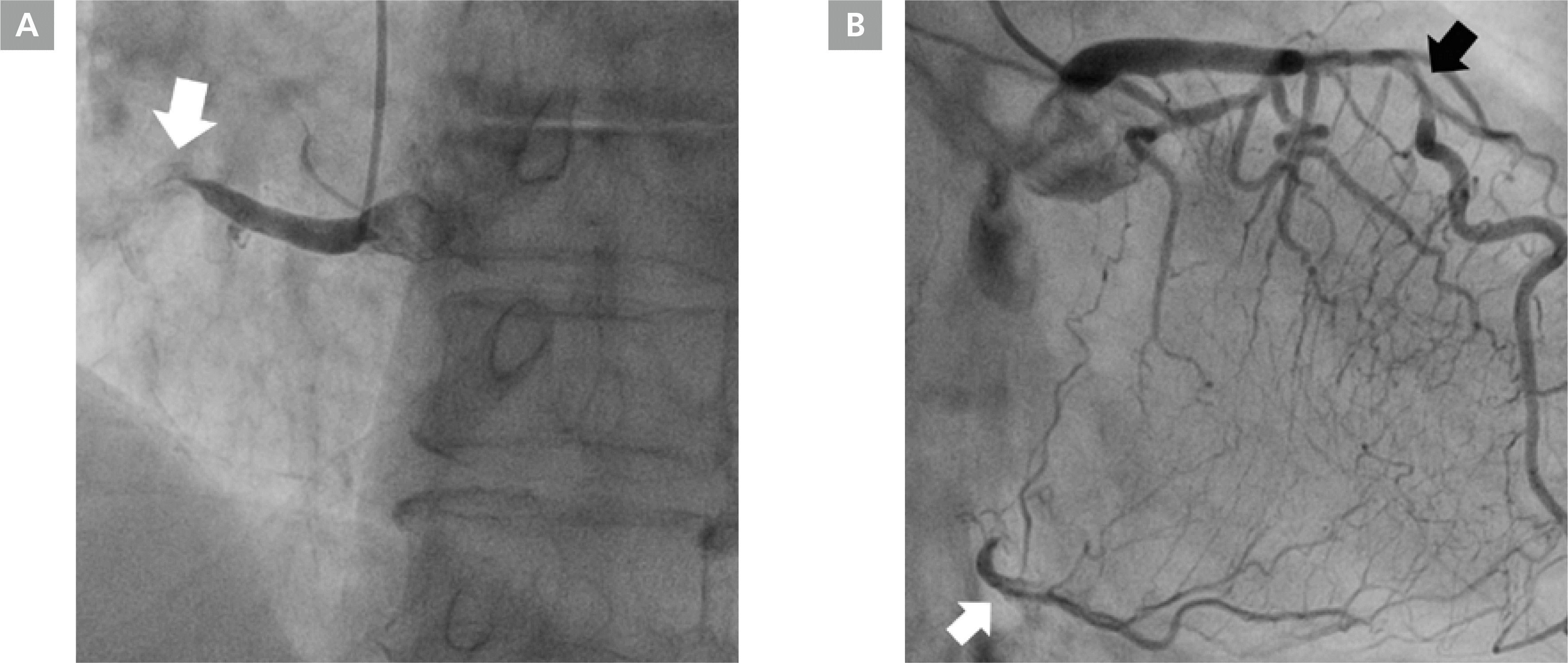
Figure 3A.
Electrocardiographic monitoring during coronary angiogram. ECG documentation of conversion from atrial fibrillation to sinus rhythm after balloon angioplasty of the occluded segment of proximal right coronary artery. 3B Final angiogram: after deployment of stents in the proximal right coronary artery, the TIMI III blood flow of RCA, sinoatrial nodal branch, right ventricular branch became apparent. ECG, electrocardiogram; RCA, right coronary artery; TIMI, thrombolysis in myocardial infarction.
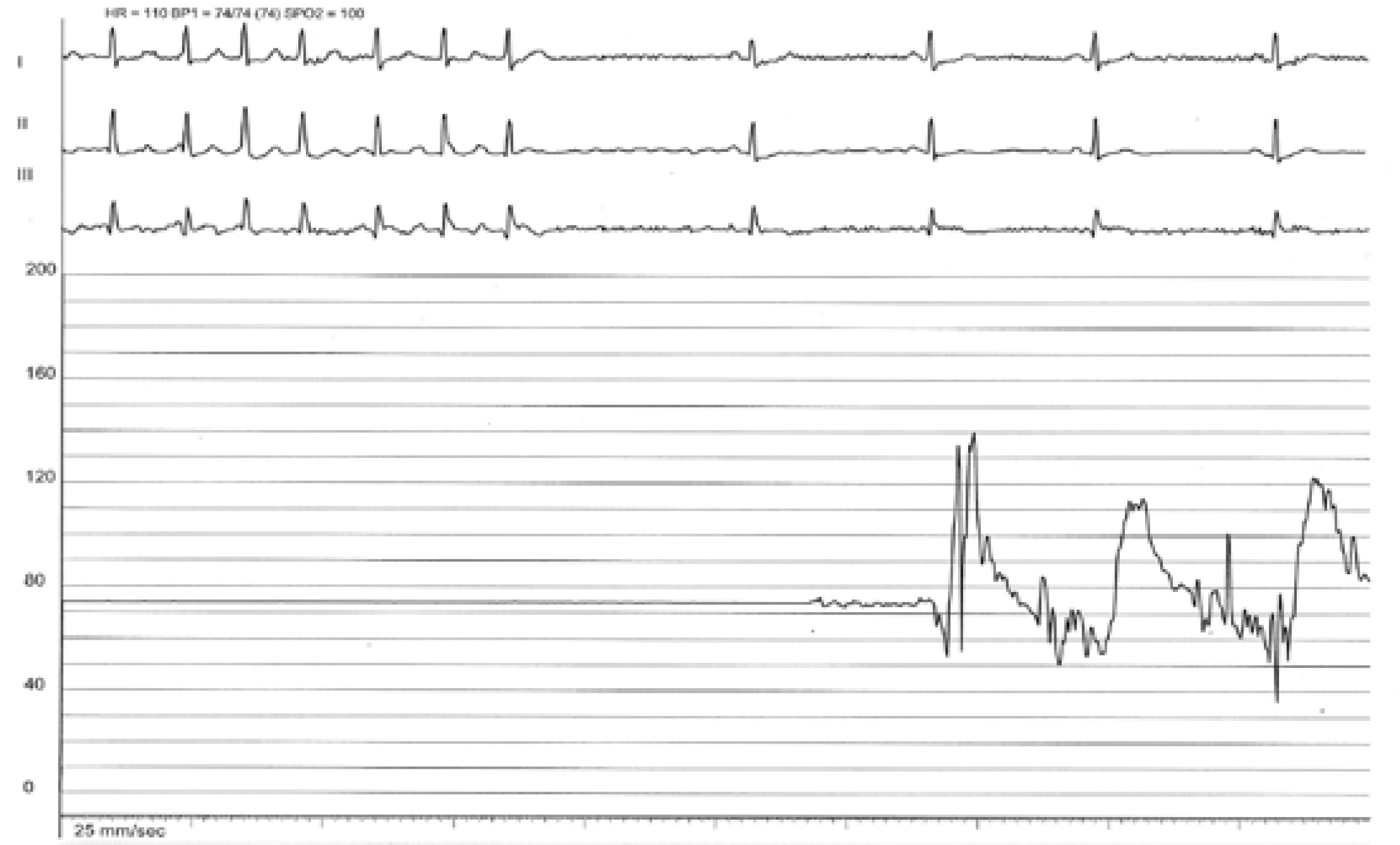
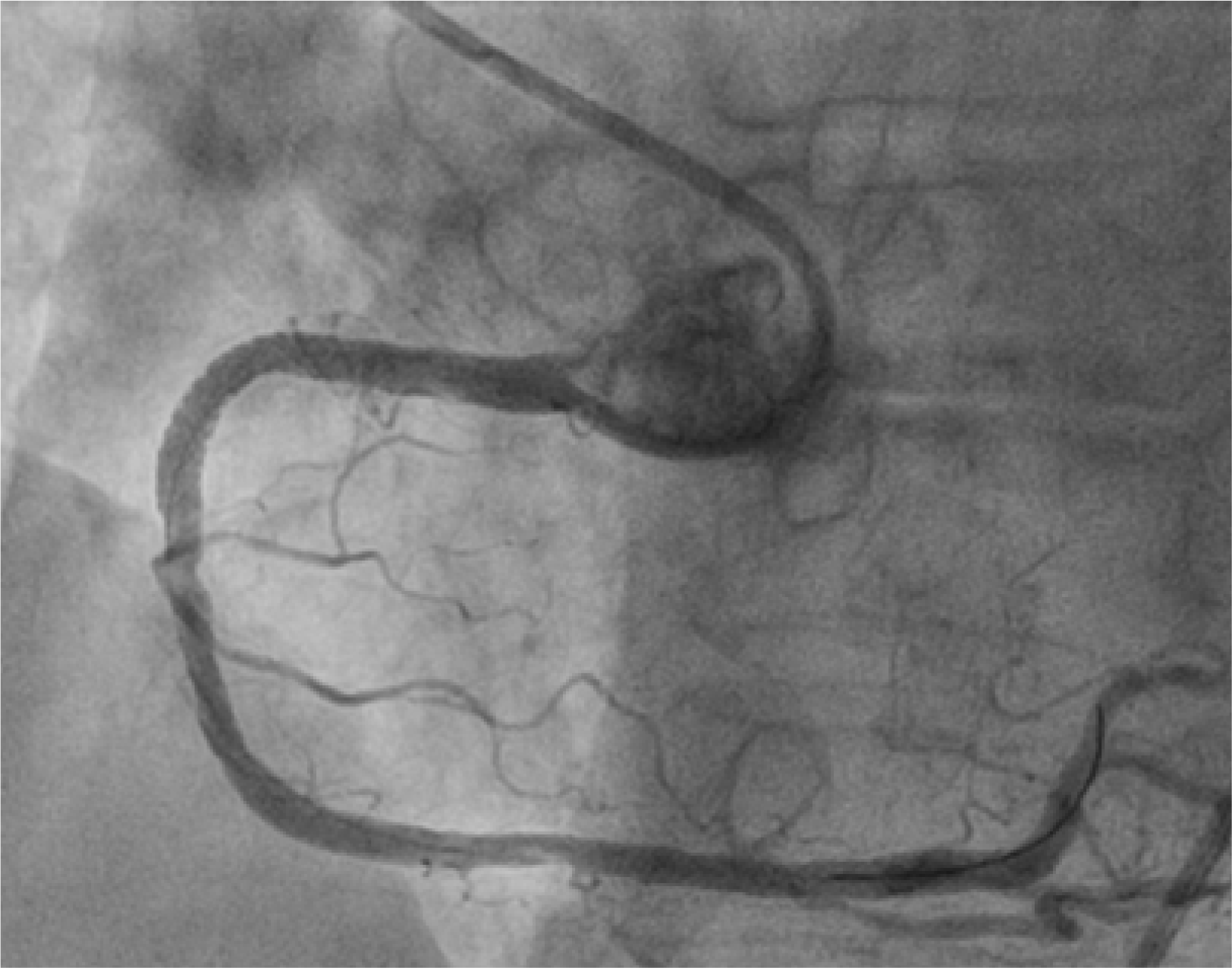
Figure 3B.
Final angiogram: after deployment of stents in the proximal right coronary artery, the TIMI III blood flow of RCA, sinoatrial nodal branch, right ventricular branch became apparent.
The patient remained in sinus rhythm throughout the duration of her hospitalization. She was subsequently discharged on a regimen of aspirin, clopidogrel, dabigatran, a β-blocker, statin, and an angiotensin-converting enzyme inhibitor. ECG, and 24-hour Holter monitoring were performed 1 month later, and no evidence of recurrent AF was found. As such, anticoagulation was carefully discontinued in favor of dual antiplatelet therapy. The patient was followed up at the outpatient department over the next 12 months. There was no evidence of AF recurrence throughout this period.
Discussion
To the best of our knowledge, this is the first report on immediate cardioversion from AF after the restoration of atrial perfusion in a patient with chronic total occlusion of the RCA.
AF is a common arrhythmia, and restoration of sinus rhythm is very important in the treatment of this condition. The pathophysiology of AF is complex and incompletely understood. Paroxysmal AF results from focal firing arising from the pulmonary veins or other sites, as well as single or multiple re-entry circuits [2]. AF may also occur when structural and/or electrophysiological abnormalities alter atrial tissue, thereby promoting the formation and/or propagation of abnormal electrical impulses. As such, any disturbance of atrial architecture potentially increases the risk of developing AF. Such changes occur most commonly in the setting of underlying heart disease associated with coronary artery disease [1].
AF is a known complication of acute myocardial infarction (MI). It occurs in approximately 10% to 20% of these patients, and is associated with more serious complications and poor long term outcomes [3,4]. Proposed mechanisms for post-MI AF include: increased LA pressure due to left ventricular dysfunction, pericarditis, increased vagal stimulation, and atrial ischemia. In patients presenting with acute ST-elevation MI and concomitant AF, atrial ischemia is believed to be the most likely cause. Hod et al. reported that 3% of patients with ST-elevation MI developed AF within 3 hours of the onset of chest pain, and that all of these cases were associated with inferior MI [5]. The authors hypothesized that atrial ischemia was the cause of AF in this context. Sakata et al. noted that successful percutaneous coronary intervention (PCI) might have an immediate effect on restoring sinus rhythm in patients with new-onset AF [6]. As such, atherosclerotic disease in atrial coronary branches may underlie the development of AF. In our patient, after the successful revascularization of the proximal RCA, the blood flow to the sinoatrial nodal branch, acute marginal branches and atrioventricular nodal branch became more apparent. These atrial branches supply atrial tissue and the sinus node along their course over the right atrium. Therefore, mechanical reperfusion of these atrial branches can potentially terminate AF and return the patient to a normal sinus rhythm. These findings support the hypothesis that atrial ischemia can cause AF, and that the mechanical reperfusion of occluded atrial branches can terminate this potentially dangerous arrhythmia.
The recurrence and duration of paroxysmal AF can result in its chronicity [7]. Structural and electrical remodeling are among the mechanisms implicated in this process. Thus, prompt revascularization in myocardial ischemia may improve the long-term prognosis of any associated AF.
Comorbid AF and coronary artery disease complicates anticoagulation and antiplatelet therapy, and is associated with higher mortality rates [8,9]. There is insufficient data to guide clinical practice optimally in such cases. Current guidelines recommend dual antiplatelet agent and anticoagulation for patients with AF after coronary artery stenting [2,10]. However, some cases of AF detected after myocardial ischemia may be short self-terminating phenomena, and thus strict adherence to the guidelines may expose these patients to an unnecessary risk of bleeding. Methods for differentiating new-onset AF from pre-existing asymptomatic AF are required. In our case, PCI resulted in immediate cardioversion. Oral anticoagulation was continued for 1 month before careful discontinuation, because the PCI was thought to have resolved the underlying cause of AF. The patient was followed up at the outpatient department over the next 12 months, and there was no evidence of AF recurrence throughout this period.














